Critical care nurses will need our support as COVID-19 cases rise
ICUs are about more than beds and ventilators – they depend on a highly skilled workforce
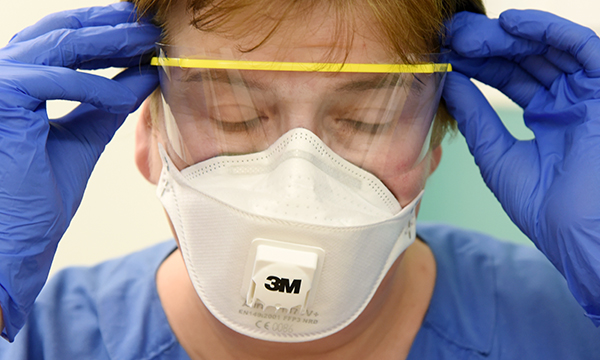
ICUs are about more than beds and ventilators – they depend on a highly skilled workforce
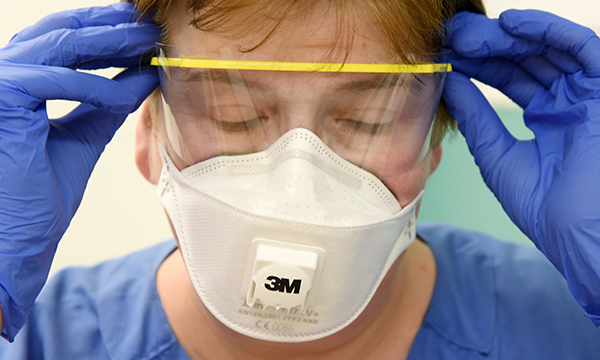
The COVID-19 pandemic has put critical care nursing in the spotlight.
It has become apparent that there is a significant lack of understanding about critical care in general and the issues facing critical care nurses.
Intensive care requires highly skilled specialist nurses
We have just over 4,000 intensive care beds in England. These beds are staffed by highly skilled and qualified specialist nurses with a nurse-to-patient staffing ratio of 1:1.
This is because patients who need to be admitted to an intensive care unit (ICU) have complex needs and require a range of highly technical interventions to support often multiple failing organ systems.
‘Nurses are scared; scared of contracting COVID-19 themselves, and of taking it home’
These interventions include invasive and non-invasive ventilation, haemofiltration, extracorporeal membrane oxygenation, inotropic management, sedation management, cardiac monitoring, arterial blood gas titration and many more.
In order to deliver this level of care safely, critical care nurses must undergo a significant amount of further training in the workplace, as well as formal academic study.
Health and social care secretary Matt Hancock pledged he would open a further 5,000 intensive care beds to help the NHS deal with patients with COVID-19.
He has talked about manufacturing more ventilators and wants retired staff back in the workforce. If we are to staff these beds with fully qualified intensive care nurses, working three 12-shifts a week, we would need to find a further 20,000. This is simply not feasible.
Nurses from other areas can assist, but not replace ICU nurses
We will need to look at redeployment of staff from other areas, such as theatres. Yet while theatre nurses and operating department practitioners are highly trained, they are not intensive care nurses and have a different skill set and expertise.
They will be able to assist, but not replace, the ICU nurse. A period of training will be required to support these staff to work in such a different environment, to protect standards of care and to ensure patient safety.
COVID-19: the impact on critical care nurses
The psychological impact on critical care staff has not yet been broached.
Nurses are scared; scared of contracting COVID-19 themselves, and of taking it home to their children, partners and relatives.
Intensive care nurses provide significant emotional support to patients and their families and this is stressful and can lead to burnout and post-traumatic stress disorder.
We need to take this issue very seriously and ensure we look after our staff as much as possible.
We have heard from nurses in Italy that managing COVID-19 patients in intensive care is made even harder when wearing personal protective equipment, which is hot and cumbersome, leading to dehydration and exhaustion.
Plan to recruit retired staff may not be a realistic option
Procuring extra ventilators is a positive suggestion. However, patients never only require the assistance of a ventilator.
What about the pumps to deliver the medication, the suction equipment, the oxygen and air needed to drive these ventilators or the cardiac monitors? Intensive care is about so much more than using a ventilator.
‘Patients with COVID-19 are in addition to, not instead of, our usual admissions’
Enabling retired staff to return to the NHS is an interesting proposition. Often retired staff are older and therefore more at risk of contracting and becoming seriously ill from COVID-19. They are more likely to have older relatives and caring responsibilities.
Equally they are under no obligation to return, so it is uncertain how realistic this is.
Our usual patient group still requires critical care
We also need to remember that while staff care for patients with COVID-19 in the ICU, we still need to manage our usual patient group, people who have had a heart attack, stroke, or who have sepsis or other medical condition. Patients with COVID-19 are in addition to, not instead of, our usual admissions.
And we work as part of a multidisciplinary team. An intensive care patient requires physiotherapy, speech and language and dietetic input.
We not only care for the physical needs of patients, but for their psychological needs and those of their families, with the critical care journey extending well beyond their ICU discharge and continuing for months and years ahead. This rehabilitation process is supported by intensive care nurses.
Critical care staff will need their colleagues’ support
We offer significant support and advice to ward staff with our critical care outreach provision. These nurses – outside an ICU environment – may find themselves managing a caseload of extremely sick patients with limited equipment and this level of skill and expertise must not be underestimated.
Critical care nursing is technical, stressful, complex, multifaceted but also hugely rewarding.
If we do not look after these critical care staff they will become unwell, depleting the workforce even further. Care, compassion and respect must extend to staff, as well as to patients in what will be extremely challenging times ahead.
 Nicki Credland is senior lecturer and head of department for paramedical, perioperative and advanced practice at the University of Hull, and chair of the British Association of Critical Care Nurses
Nicki Credland is senior lecturer and head of department for paramedical, perioperative and advanced practice at the University of Hull, and chair of the British Association of Critical Care Nurses
