Call for healthcare staff exemptions after long-term permits were deemed invalid
How to
Image

Understand important areas to consider when assessing patients’ mental capacity
Image

Strategies to reduce errors, including enhanced training, double checking and use of AI
Image

Keep your knowledge of guidance on the management of suspected sepsis up to date
Image
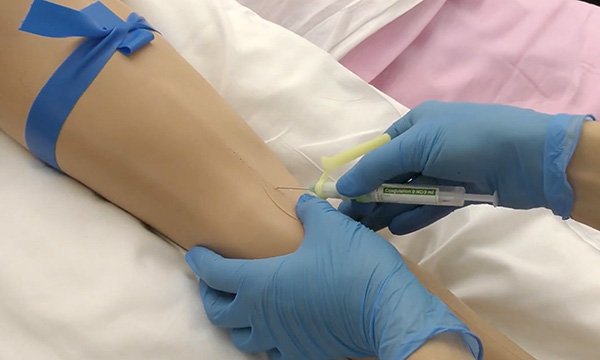
It must be done correctly to prevent any misleading blood test results
Image
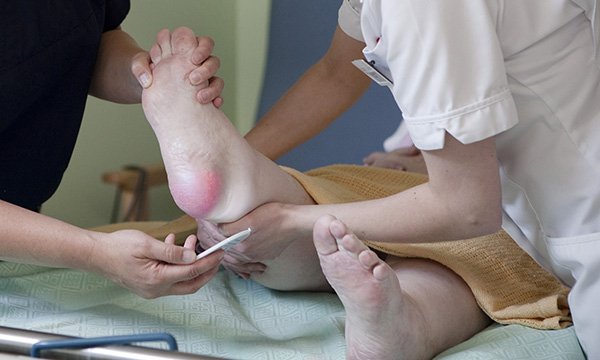
Learn how to distinguish pressure ulcers from other types of skin damage
Image
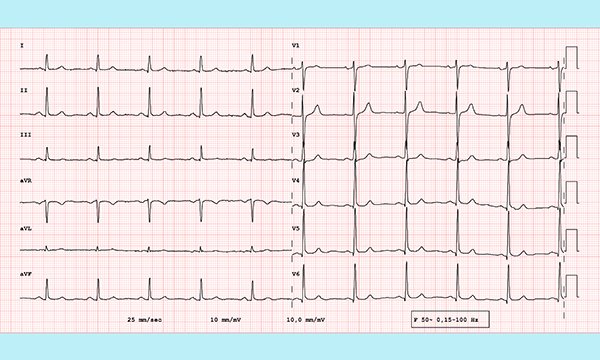
Learn about issues that might lead to inaccuracies when undertaking a recording
Image
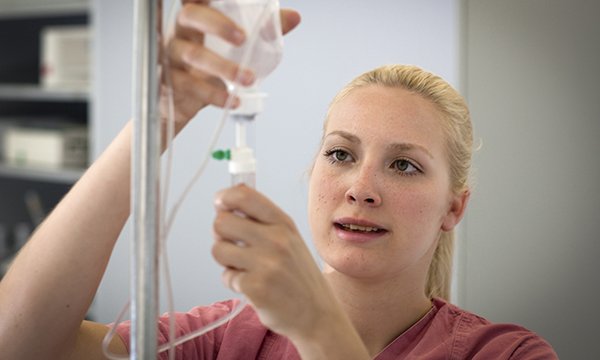
Enhance your understanding of aseptic technique when performing this procedure
Image

Learn how to present a structured business case to optimise its chance of success
Image
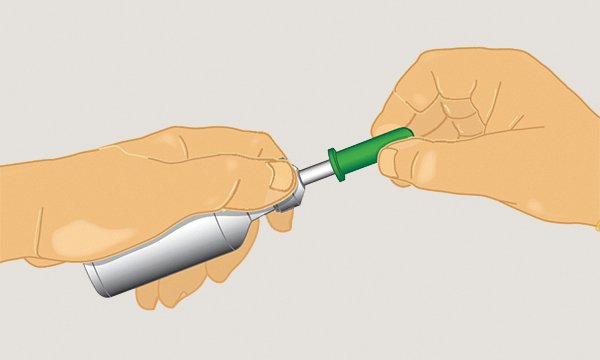
Familiarise yourself with the procedure and its potential risks and complications
Image

Recognise the complexity of medication errors and the importance of adhering to protocols
Image
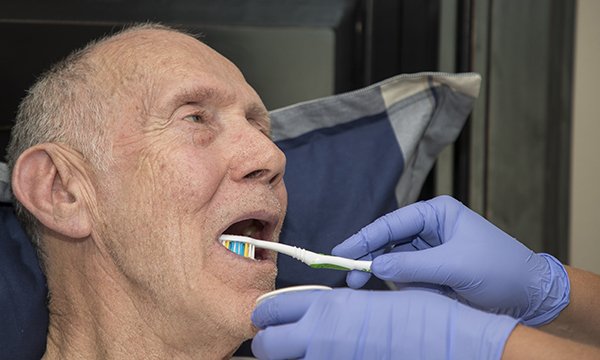
Understand the preparation, equipment and procedure involved to ensure optimal oral health
Image
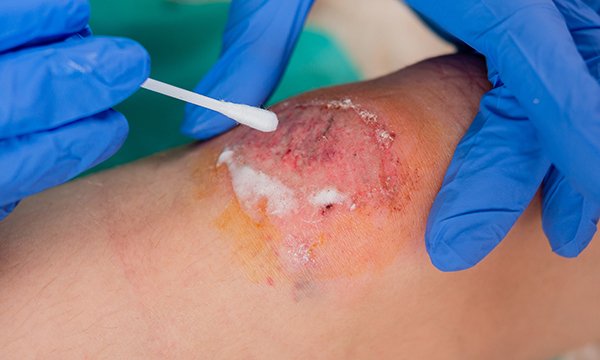
Refresh your knowledge of the preparation and procedure for obtaining a wound swab safely
Increase your knowledge of quality improvement and read a step-by-step guide
Enhance your awareness of the signs of localised, spreading and systemic wound infections
Increase your knowledge of common applications of local anaesthetic during or after surgery
Understand the procedure and the indications and contraindications for their use
Recognise the associated complications and the importance of infection prevention and control
Familiarise yourself with the tools you can use to explore a person’s pain experience
