End of life care in a pandemic: the emotional cost to nurses
I have seen first-hand how nurses rise to the challenge – but they must be offered support
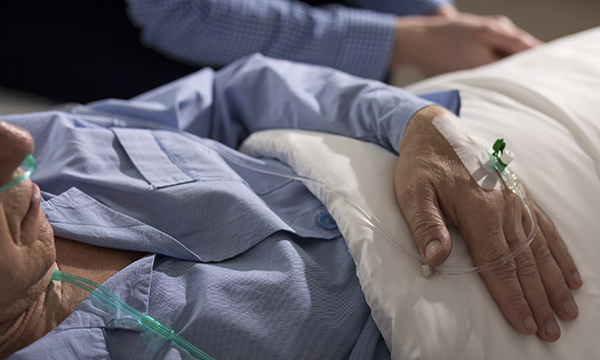
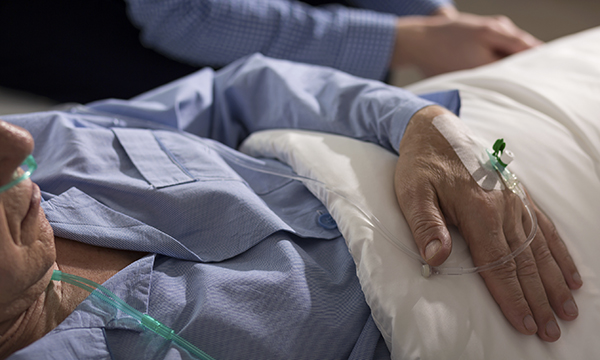
Nurses caring for dying patients have told us of the burden of PPE, and the role they play in the absence of loved ones
Findings of our annual end of life care survey, now in its fourth year and conducted in partnership with charity Marie Curie, always make for sobering reading.
In ‘normal times’, the accounts from nurses offer real-life insights into how staffing and time pressures hamper the care of dying patients.
These issues haven’t gone away of course, but in this extraordinarily challenging year so many more have been added into the mix, causing emotional distress for many nurses.
Impact of wearing PPE while caring for dying patients
The term ‘barrier to care’ became literal this year, with universal use of personal protective equipment (PPE) now being essential. This was singled out by 33% of the almost 900 survey respondents as the biggest factor getting in the way of care of dying patients.
‘Nurses who sat alone with patients in their final hours told us they absorbed the emotions of the death and had to shoulder that ‘huge responsibility’ on behalf of families’
PPE even out-does staffing levels as the main obstacle to end of life care in 2020, according to our survey. Last year, 65% of respondents reported staffing as being the main barrier to end of life care, compared with 15% this year.
The emotive issues nurses must navigate with patients’ loved ones
This year’s survey has personal resonance for me because I lost my dad in April, at the height of the first wave of the pandemic. I recall a hospice nurse telling me that giving care from behind PPE was ‘just not how we do things’. And yet, somehow, this nurse managed to do an outstanding job of making dad as comfortable as possible.
In common with nurses in this survey, those caring for my father had to ask some painful questions of relatives, such as in our case, which of his four children would see him. I honestly don’t know whether this was more awful for us or for those compassionate staff members.

Some employers are better than others at supporting nursing staff
Nurses who sat alone with patients with COVID-19 in their final hours told the survey they felt they absorbed the emotions of the death and had to shoulder that ‘huge responsibility’ on behalf of families.
So as we contemplate the shifting phases of this pandemic, we must ask what can be done to protect nurses’ well-being.
There is no easy answer and some employers are better at providing support than others.
In a welcome move, NHS England and NHS Improvement has pledged rapid access to mental health services with specific support for those working in critical care. This, says chief nurse Ruth May is in direct response to feedback from nursing staff.
There are a number of national, local and virtual services specifically for nurses and we will continue to promote those via our free-to-access COVID-19 resource centre. We will be publishing an article on this very soon.
The ongoing challenges of the pandemic will mean nursing staff must continue to draw on the mutual support of colleagues and teams. As nurses know all too well, this comes at personal cost – one that employers and governments must do everything they can to minimise.
COVID-19 resource centre

