Proactive education for young people as they learn to self-manage long-term conditions
Evidence and Practice

Proactive education for young people as they learn to self-manage long-term conditions
A study suggests ways to develop strategies to help prevent, detect and manage anxiety
It must be inclusive, supportive and aligned to the needs of children and young people and their families
Clinical

A study suggests ways to develop strategies to help prevent, detect and manage anxiety
It must be inclusive, supportive and aligned to the needs of children and young people and their families

Enhancing nurses’ understanding of extra-familial harm and contextual safeguarding

Nurses need more education on the care of autistic children and young people and their parents

How virtual resources can support nurses and children and young people in conflict settings
CPD articles

Symptoms and pathophysiology of APBS and the importance of a multimodal management strategy

Lessons from failures, barriers nurses may face and strategies to maintain child-centred practice
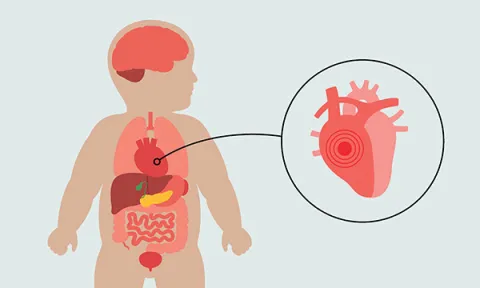
Improving nurses’ recognition of symptoms that may indicate a serious cardiac condition
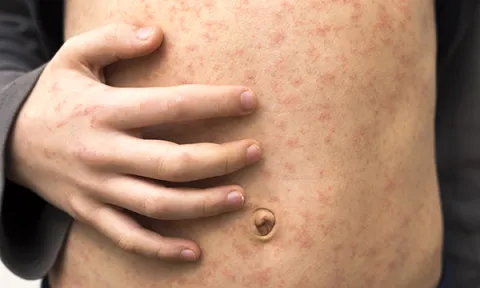
The epidemiology of measles and the measles, mumps and rubella vaccine
Second of two articles that aim to develop nurses’ understanding of SPOT programme and PEWS charts

How nurses can identify and document deterioration in a child’s health status
Practice question
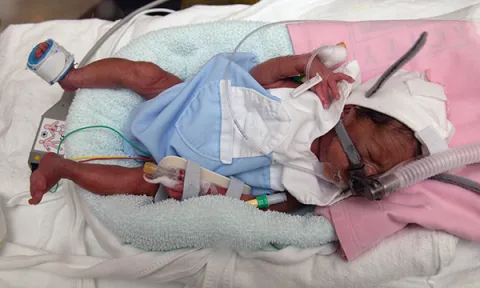
Why CPAP is used, complications, and how it differs from non-invasive ventilation (NIV)

ECMO can support children with primary respiratory and cardiac failure

Good communication is essential to elicit accurate information and optimise care

Young people should have access to education, assessment and treatment for sexual health

Children undergoing bone marrow transplants need support and follow up

Children’s nurses can help prevent young people from being exploited in drug trafficking
A to Z of syndromes

First identified in 2015, there is no vaccine for this virus, which can have devastating effects on the unborn child
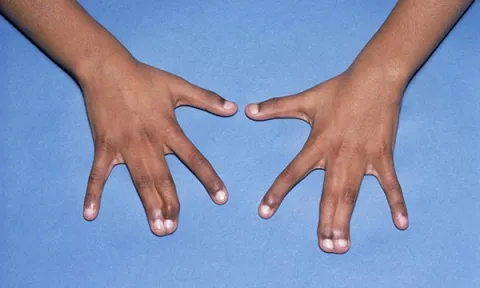
An insight into this rare genetic disorder in which both parents are recessive gene carriers
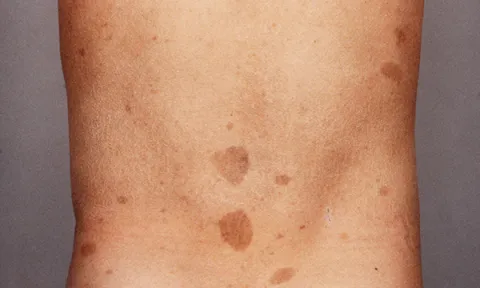
An insight into this genetic disorder occurring in 1 in 6,000 infant males

Waardenburg syndrome is a genetic disorder that gives people a distinctive appearance

Understanding Usher syndrome which is found in approximately 10,000 people in the UK
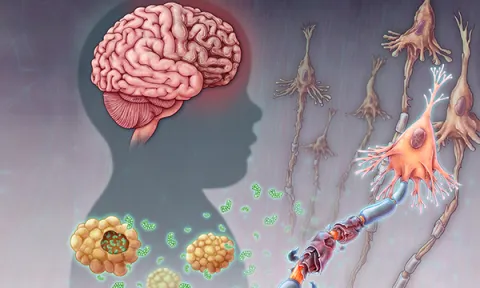
An insight into this genetic disorder which carries a poor prognosis and is often fatal

