PORTFOLIO USERS:
Please be aware that we are doing a security upgrade on our website between 11 - 14 May. During this time you can view your Portfolio dashboard and download your main Portfolio PDF, but you will not be able to add anything new to your Portfolio. This necessary maintenance helps keep your data safe and secure. We are sorry for the inconvenience and thank you for your patience.
A to Z of syndromes
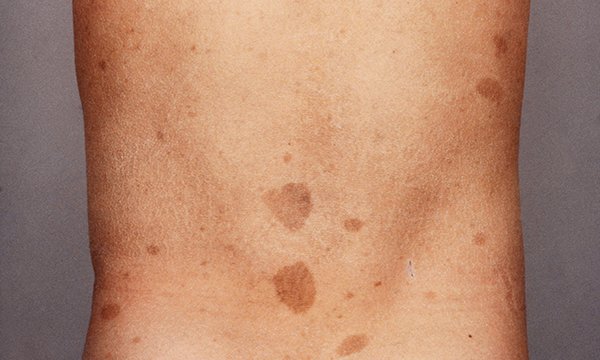
A-Z of syndromes: X-linked ichthyosis
An insight into this genetic disorder occurring in 1 in 6,000 infant males
Posted 01 February 2019 - 12:26
Posted 01 February 2019 - 12:26
Jobs
Related articles
Baby death leads to renewed call for regulation of ‘nurse’ title
Grandson of Steve Bruce died after being placed in ‘unsafe position’ by worker hired as nurse
24 Mar 2026
Risk factors and nursing interventions for non-traumatic fractures in neonates and...
Children’s bone fragility and the critical role of nurses in identification and prevention
23 Feb 2026
Childhood arrhythmias: diagnosis, management and nursing care
Improving nurses’ recognition of symptoms that may indicate a serious cardiac condition
24 Nov 2025
Free
How can children’s nurses help to increase childhood vaccination uptake?
Work needs to be done in communities to help unpick the reasons for vaccine hesitancy
11 Jun 2025
5 Most Read Articles
Top-rated nurse employers named: what makes a great workplace?
The highest scorers in the NHS Staff Survey, based on flexible working, morale and more
11 May 2026
Six reflective exercises to help improve your communication skills
Steps for building better communication with patients and colleagues
22 Apr 2026
Your annual appraisal: how to prepare and what to expect
Tips to ensure your appraisal reflects your contributions, plus how it’s linked to pay
30 Jan 2025
Nurses’ actions before patient’s suicide amounted to gross failures of care and neglect
Coroner criticises failures to check patient record before tragedy, the latest at the trust
08 May 2026
NHS band 5 role reviews and potential for pay uplift: your questions answered
Q&A on who is included, why rethink of nurses’ bandings is needed and when reviews start
17 Apr 2026
