Your views
Letter from Zambia 6: Different ways of training
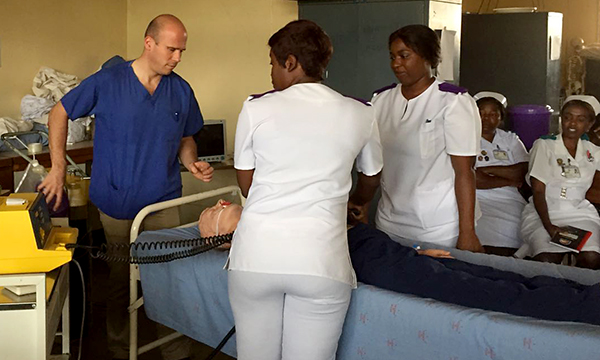
Since 2014, nurses and nursing students from the UK have been visiting Zambia and working with the Ministry of Health there to help develop critical care nursing. Here a group of students describe how their counterparts are trained in Zambia and find major differences from the UK system.
Image