Nicola Ranger says nurses may strike locally against trusts that resist band 5 pay increase
CPD articles
Image

Refreshing nurses’ knowledge of the pathophysiology, assessment and management of haemorrhage
Image

Emergency nurses’ understanding of the patient safety incident response framework (PSIRF)
Image

Exploring ways in which handover delays can be addressed by emergency department nurses
Image
Professional learning designed to suit your busy schedule
Image
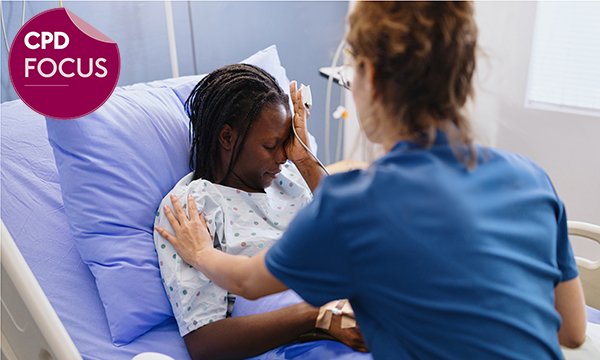
Refreshing ED nurses’ knowledge of the pathophysiology and signs and symptoms of sepsis
Image

The aetiology and signs and symptoms of adults with type 1 and type 2 diabetes
Image
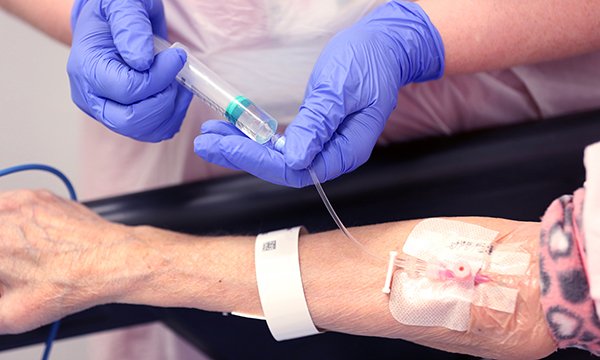
Nurses' role in patient education on signs and symptoms of DVT and PE and rationale for thromboprophylaxis
Image

Using a triage algorithm and clinical reasoning to support decision-making in the ED
Image

A prognostic model predicting complications helps nurses to asses risk and level of care required
Image

How nurses can manage patients' expectations in a busy and unpredictable environment
Image

The unique challenges of having to care for patients in non-clinical areas
Nurses working in EDs can help ensure that the care needs of dying patients and their families are addressed
Overview of epidemiological perspectives including the nurse’s role in antibiotic stewardship
Familiarise yourself with frailty screening tools often used in emergency care settings
This can be achieved by nurses developing cultural knowledge and interpersonal skills
Understand how to assess and manage patients with vaso-occlusive crisis in the ED
Preparing autonomous practitioners to break news of serious and new diagnoses

