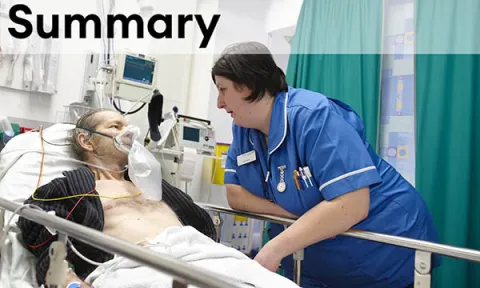
Importance of effective communication and shared decision-making to support safe patient care
Evidence and Practice

Importance of effective communication and shared decision-making to support safe patient care
Outlining steps nurses can take to mitigate some of the associated risks of an overcrowded ED
Clinical

Outlining steps nurses can take to mitigate some of the associated risks of an overcrowded ED

Emergency nurses’ important role in recognising unmet need related to dental neglect
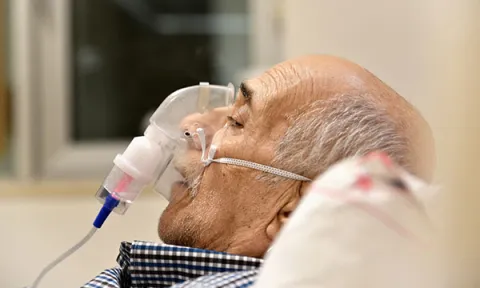
A look at the equipment and preparation required for NIV as well as the procedure and evidence base
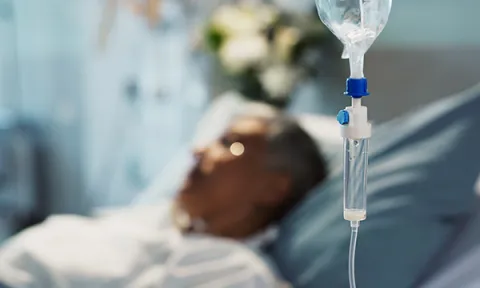
Quality improvement project aimed at patients with suspected neutropenic sepsis

Need for systemic change including reflection time, peer support and compassionate leadership
CPD articles

Refreshing nurses’ knowledge of the pathophysiology, assessment and management of haemorrhage

Emergency nurses’ understanding of the patient safety incident response framework (PSIRF)

Exploring ways in which handover delays can be addressed by emergency department nurses
Professional learning designed to suit your busy schedule
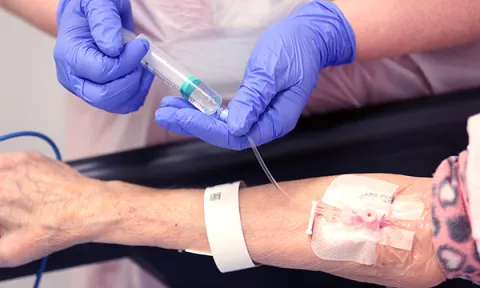
Refreshing ED nurses’ knowledge of the pathophysiology and signs and symptoms of sepsis
How to

Tips for nurses on preparation, equipment, procedures to follow and where to find resources

The importance of taking a patient history effectively as part of the diagnostic process

Familiarise yourself with the steps required when triaging a patient in the ED

A step-by-step framework nurses can use when having challenging conversations

Mistakes made in healthcare settings and the challenges to staff that arise from them can harm service users, consume time and money, and often receive bad publicity. However, by...
Practice question

Ambulance patient handovers are time-critical, complex processes vital for patient outcomes

Be vigilant to spot traumatic injuries, with a low threshold for escalation

Practical steps nurses can take to ensure everyone’s safety

Advice on recognising burnout in yourself and others, and where to find support
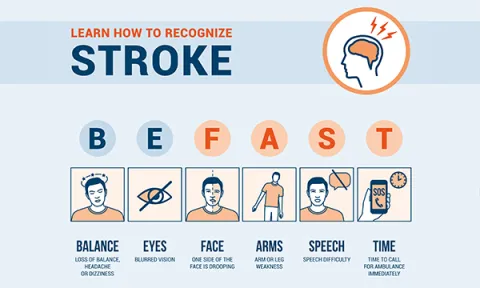
It can be difficult to recognise the symptoms, but the BEFAST acronym can help

Even short conversations about weight can help patients, but avoid suggesting blame