The impact of a four-week elective primary care placement on preregistration nursing students
Evidence and Practice

The impact of a four-week elective primary care placement on preregistration nursing students
High-quality trainee AP guidance is crucial for professional development and patient safety
Learn about the frequent challenges experienced by service users and healthcare providers
Clinical

High-quality trainee AP guidance is crucial for professional development and patient safety

Learn about the frequent challenges experienced by service users and healthcare providers

Exploring the variation in the support available to advanced practitioners across the UK

Barriers include inconsistent delivery, variable relationships and insufficient support

The use of artificial intelligence in areas such as nursing documentation and wound care
CPD articles

This article aims to support community nurses by simplifying the selection of compression hosiery
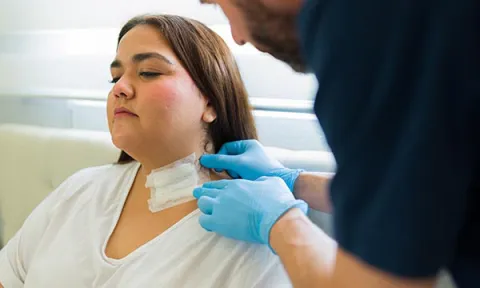
Aiding primary care and community nurses to assess and manage post-surgical wounds

Strategies for incorporating CVD prevention and management into routine COPD care

Supporting patients with coexisting CVD and mental health conditions in primary care

Professional learning designed to suit your busy schedule
Research focus

Primary care nurses need to be able to identify and manage self-harm. This research focus explores high risk groups and management strategies

Three studies highlight the complexity of this disorder – and the provision of treatment

Three recent studies look at methods to facilitate greater integrated care

Three studies highlight the growing incidence of eating disorders in primary care
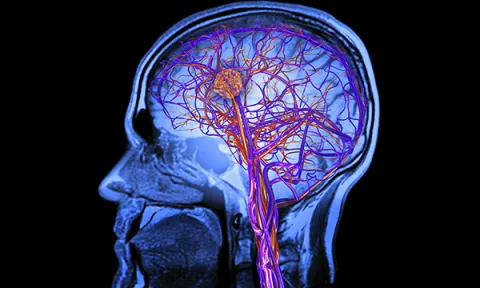
Rehabilitation for upper limb impairment, which occurs in a majority of strokes, is reviewed

Three studies examine the benefits of music-based therapies for people with dementia


