Coroner criticises failures to check patient record before tragedy, the latest at the trust
Clinical
Image

Can the lived experience of migration be drawn on to promote healthy ageing?
Image

Ways in which nursing and care home staff could support older people with hearing loss
Image

Surface-acted empathy can function as a compassionate tool but should not replace empathic engagement
Image

How an Admiral Nurse service implemented a care pathway in Cornwall and the Isles of Scilly
Image

How a nurse and physiotherapist hospital model provides acute care for older adults
Image

Understanding key steps can help nurses feel confident to change their practice
Image
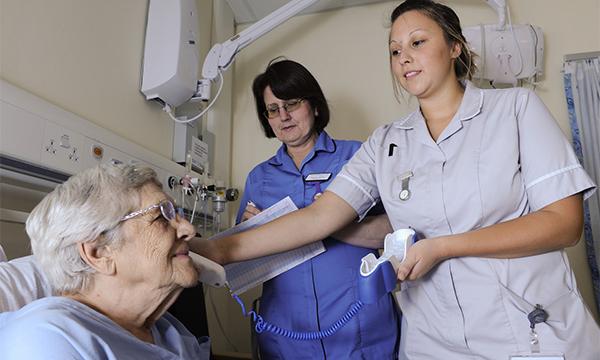
Targeted initiatives can foster more positive attitudes towards this field of practice
Image
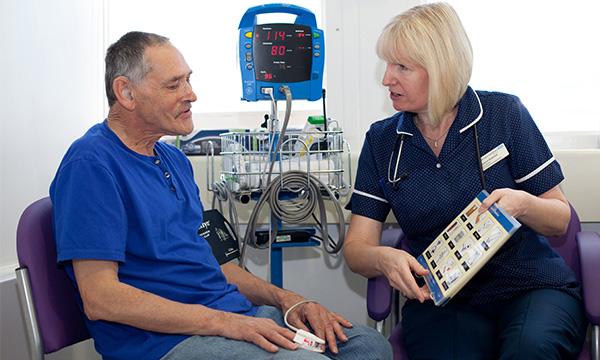
Essential nursing considerations when caring for this patient group in the ED
Image

Review highlights need for holistic care addressing physical, psychological and social influences
Image

How nurses can create an enabling environment by using person-centred communication techniques
Image

Better pain assessment tools and training needed in caring for people with dementia
Nurses’ understanding of best interests decision-making in the context of dementia care
Risks for older people experiencing a ‘long lie’ after a fall in pre-hospital services
Identifying pain and other symptoms of long-term conditions in older people with dementia
Study exploring the challenges when providing care in acute general hospital settings
Simulation allows students to develop skills which might be difficult in clinical settings
Your quick-read article summary

