Importance of early introduction, clear communication, accessibility and a holistic approach
Evidence and Practice

Enhancing nurses’ understanding of the effects patients can experience after radiotherapy
Importance of early introduction, clear communication, accessibility and a holistic approach
Strategies nurses can use to support prevention, assessment and treatment of nail toxicities
Clinical
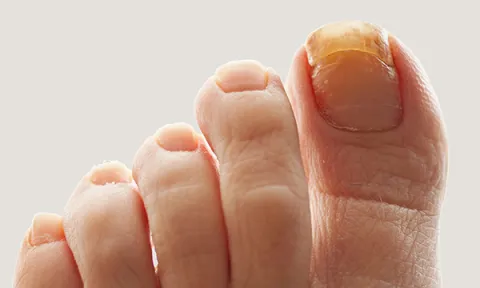
Strategies nurses can use to support prevention, assessment and treatment of nail toxicities

A service evaluation of patient satisfaction with the clinic and whether it met their educational needs

Nurses should offer support to self-manage tailored to patients’ health status, needs and preferences

How early diagnosis could be supported by campaigns to recognise signs of bowel cancer
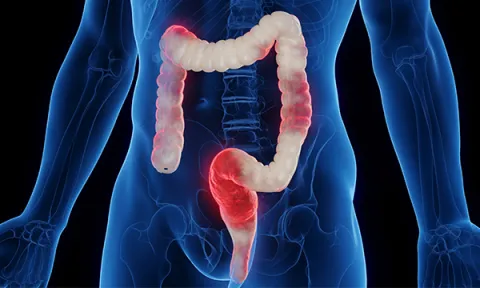
Patients must be systematically assessed with thorough investigations to reach a correct diagnosis
Clinical

Enhancing nurses’ understanding of the effects patients can experience after radiotherapy

Early identification of frailty followed by referral for a comprehensive geriatric assessment

Nursing teams must identify and address patients' needs before, during and after treatment

Radiotherapy can affect physical, psychological and social functioning

Non-pharmacological approaches, what matters to patients and families and nurses' self-care are key
Practice question

Clinical nurse specialists are pivotal – but they also need support to maintain expertise

By focusing on what matters to patients, personalised care can provide more choice

Promoting trusting relationships and using available resources can help conquer patient fear

Cancer services for people with dementia must be organised, flexible and offer continuity

Exploring the personal meaning of pain for patients can help with support and treatment

Tips and advice for nurses caring for people with cancer during the pandemic


