
A must-have book that sets out the main concepts of law and ethics in healthcare.
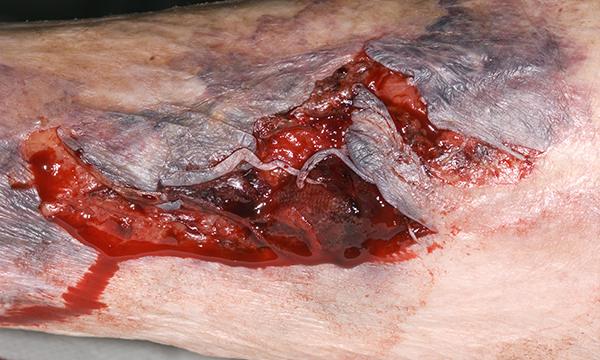
Skin tears are common in older people. They are acute wounds that are at high risk of becoming complex, chronic wounds due to the interplay between the physiological changes in the skin and trauma from the external environment. Skin tears have been reported to have prevalence rates equal to, or greater than, those for pressure ulcers. A comprehensive risk assessment should include assessment of the individual’s general health (chronic/critical disease, polypharmacy and cognitive, sensory and nutritional status); mobility (history of falls, impaired mobility, dependent activities of daily living, and mechanical trauma); and skin (extremes of age, fragile skin and previous skin tears). A recognised classification system should be used to identify and document skin tears and guide treatment decisions in line with local wound management protocols. Nurses and carers are in a prime position to prevent, assess and manage skin tears.
Accurate and considered wound assessment is essential to fulfil professional nursing requirements and ensure appropriate patient and wound management. This article describes the main aspects of holistic assessment of the patient and the wound, including identifying patient risk factors and comorbidities, and factors affecting wound healing to ensure optimal outcomes.
An ‘all-in-one’ guideline on pressure ulcer prevention and management in primary and secondary care was published last year by the National Institute for Health and Clinical Excellence (

The reality of wound management in clinical practice leaves a lot to be desired in relation to dressing selection and use. Maureen Benbow highlights some of the problems currently being encountered in relation to good wound management practice and illustrates good practice with a particularly difficult case study.
A basic understanding of patient assessment, wound assessment, dressing properties and their appropriateness at different stages of healing and for differing clinical appearances is essential to achieving success in wound and patient management. The author uses an unusual case study to illustrate the thinking and informed decision-making behind the choice of dressings used in combination.
The issues to be addressed in relation to the management of wounds generally reflect the professional accountability of nurses and how they try to avoid harming the patient, the cost implications of dressings, their efficacy and clinical effectiveness and how practice can be improved.
