
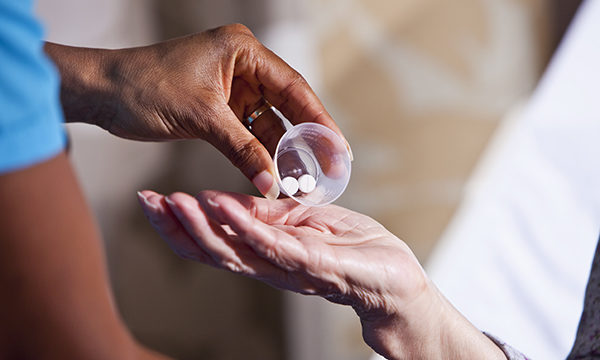

We work in the residents' home, they don't live in our workplace, says the head of nursing at Four Seasons Health Care.

This article, the second of two, provides healthcare practitioners with an overview of best practice in palliative and end-of-life care, including nutrition, hydration, oral hygiene and pain management. Communication and spiritual care are discussed, as well as care after death. Providing support and education for families is an important aspect of palliative and end-of-life care. Care home nurses should ensure that the person living with dementia is at the centre of decision making, and provide care that is inclusive of their needs and wishes. The article is framed in a care home context; there is little research about how to optimise palliative care for people living with dementia in care homes
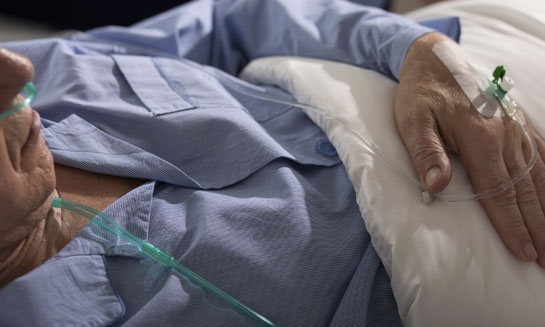
The terms palliative and end of life care are often used interchangeably and healthcare practitioners may perceive that palliative care is only appropriate during the terminal stages of an illness. This article, the first of two parts, provides healthcare practitioners with an overview of the concept of palliative care. It explains how this can be differentiated from end of life care and how it should be commenced in a timely manner, so that people who are living with dementia can contribute to the planning of their future care and death. The policies and tools used in the provision of palliative and end of life care are discussed, including advance care planning and The Gold Standards Framework. The article is framed in a care home context; there is little research about how to optimise palliative care for people living with dementia in care homes. The second part of this article will discuss end of life care and the best practices for providing end of life care, including nutrition and hydration, oral hygiene, pain management and spiritual care.
The term ‘named nursing’ was introduced in the UK more than 25 years ago but it has re-emerged recently in the light of recommendations made in the Francis report on the poor standards of care at Mid-Staffordshire NHS Foundation Trust. The original definition of named nurse by the Department of Health was someone that a patient could identify as responsible for their care from hospital admission to discharge. It was largely practised in the UK exclusively but there are now various accounts of its use throughout Europe, particularly Scandinavia, and North America.
This article provides an overview of the named nursing concept. It provides recommendations for implementation of a named nursing system in nursing home settings, because most previous recommendations have referred to acute hospitals.
