Image

Nurses should help parents get access to the safe and effective vaccines for their children
26 Feb 2024
Image

A description of a children’s hospital journey towards Pathway to Excellence accreditation
17 Aug 2021
Image

Placements of this type can help students appreciate the role of public health in nursing
21 Jul 2021
Image

As the vaccination programme gets underway, nurses step up again
09 Dec 2020
Image
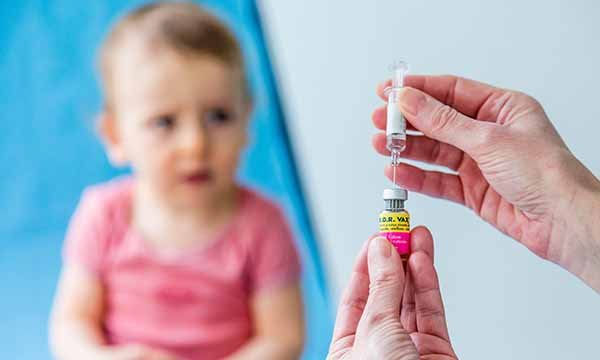
What to consider so childhood vaccination clinics continue and parents are supported
30 Sep 2020
Image
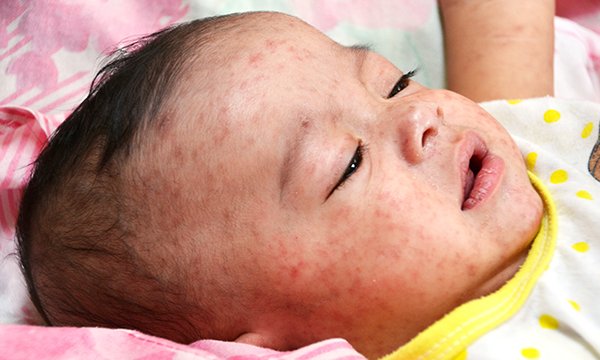
13 Sep 2019
Image

A funding complication could result in some public health nurses leaving
13 May 2019
Image

17 Oct 2018
Image
17 Jul 2018
Image
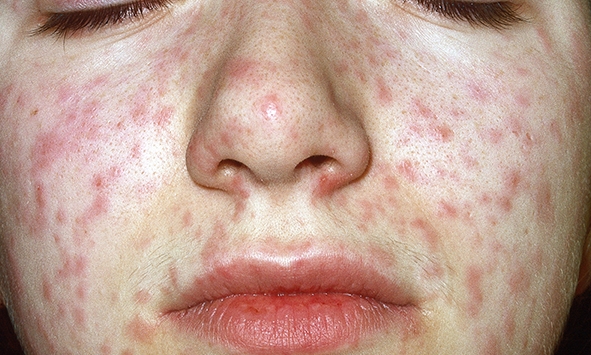
11 Jul 2018
Image

27 Sep 2017
Image

Carmel Bagness and Helen Donovan, who are leading the RCN’s online resources on domestic abuse, explain what you need to know to identify and support victims
19 Oct 2016
01 Nov 2013
01 Jul 2013
01 May 2013