




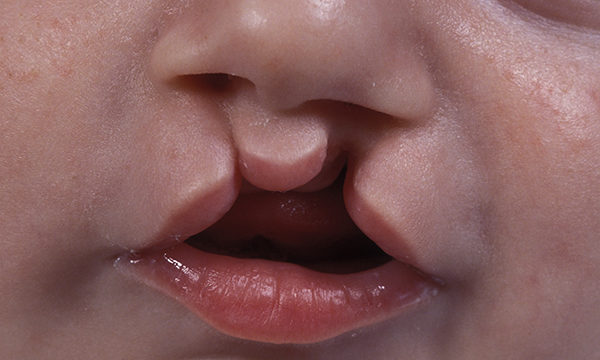
A series about conditions with common symptoms that constitute a syndrome
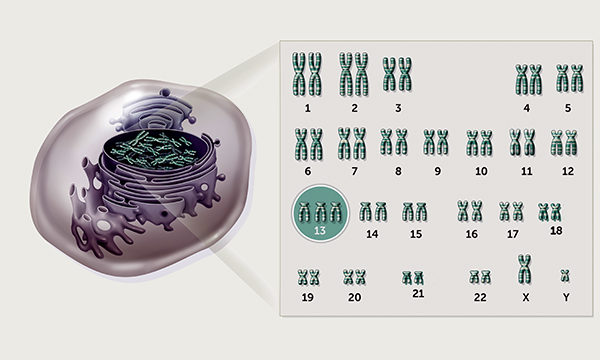
A series about conditions with common symptoms that constitute syndromes

Continence is regarded as a basic need and many continence problems can be addressed and managed effectively. People with an intellectual disability (ID) are at greater risk of developing urinary incontinence (UI), however action to address their needs is minimal and the quality of care they receive varies despite national care standards and guidelines. This article examines promotion of continence in people with an ID and explores the literature on assessment and management of need. It also discusses the factors ID nurses should consider when meeting the continence needs of people with an ID, including explaining important terms, and assessing and managing UI and continence promotion, as well as their role in providing care and support in a person-centred and inter-professional context.
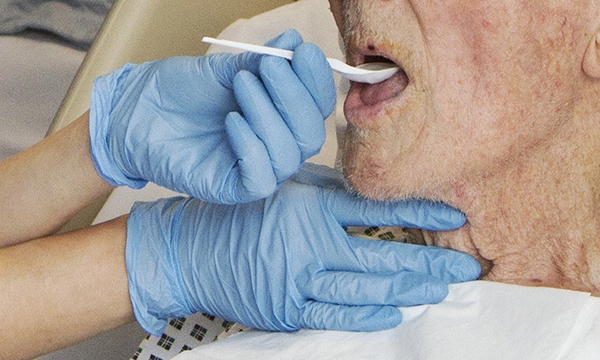
This article outlines the difficulties that people with severe and profound intellectual and multiple disabilities may have when swallowing. The article explains the prevalence, causes and nature of swallowing difficulties for people with intellectual disabilities and discusses the assessment of swallowing, eating and drinking problems. It also examines management of swallowing problems in this cohort, and uses a case study to consider how to support someone with such difficulties in the context of Orem’s self-care deficit theory. The article concludes with broad recommendations for care.
This article outlines the difficulties that people with severe and profound intellectual and multiple disabilities may have when swallowing. The article explains the prevalence, causes and nature of swallowing difficulties for people with intellectual disabilities and discusses the assessment of swallowing, eating and drinking problems. It also examines management of swallowing problems in this cohort, and uses a case study to consider how to support someone with such difficulties in the context of Orem's self-care deficit theory. The article concludes with broad recommendations for care.
Increased life expectancy allied to increasing numbers of people with learning disabilities living in the community means that more people with learning disabilities are having their health needs met in acute general medical services. In the context of a person-centred approach, this article examines the potential problems that may arise in all healthcare settings which pose barriers to effective healthcare delivery. These include perceptions and attitudes of healthcare staff, issues of consent and communication. It proceeds to outline solutions that enable these barriers to be overcome. Such solutions centre around addressing communication difficulties and issues of consent as well as developing the education of healthcare professionals. It concludes with a case study that explains how the theoretical principles may be applied sensitively in a practice situation.