Rebecca Myatt
Understanding oral mucositis and the principles of effective mouth care
Recognise the symptoms, causes and risk factors, and the importance of optimal oral hygiene
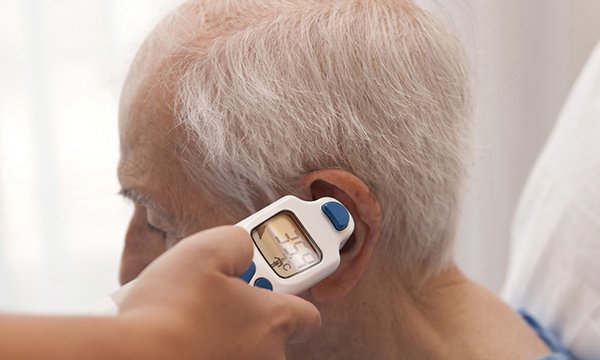
How to take a patient’s temperature
A step-by-step guide to the procedure using the oral, tympanic, axillary and forehead sites
X-rays: what the nurse needs to know
Rationale and key points X-ray imaging is a form of electromagnetic radiation that is able to pass through the human body producing an image of the internal structures. X-rays are one of the main investigations for confirming a suspected diagnosis. Developing an understanding of the underlying mechanism and the rationale for requesting an X-ray will increase nurses’ understanding of the process and enable improved patient preparation through explanation and reassurance. This article provides an overview of the fundamental principles underlying the process of obtaining an X-ray. » X-ray imaging is a common diagnostic tool that nurses will encounter on a regular basis. » Several factors affect the production of a clear X-ray image, including patient movement. » Radiation safety and avoidance of unnecessary exposure are paramount. » Co-operation and communication by the multidisciplinary team are vital to ensure that X-ray imaging can be requested, performed, interpreted and acted on, and the findings communicated to the patient.
Pulse oximetry: what the nurse needs to know
Rationale and key points Measurement of peripheral oxygen saturation (SpO 2 ) is used to identify early hypoxia in patients and evaluate the effectiveness of oxygen therapy. Nurses should be aware of the procedure for using a pulse oximeter to measure SpO 2 levels and the normal range for SpO 2 readings. » A pulse oximeter is used to measure SpO 2 levels, and involves placing a probe on the patient’s finger, toe or ear lobe. » A SpO 2 level of less than 90% is a clinical emergency. If the SpO 2 level is below 94%, the nurse should assume the patient is hypoxic until proven otherwise, and therefore they may require supplemental oxygen administration. » Nurses should be aware of the factors that might affect SpO 2 readings, including anaemia, peripheral vasoconstriction, dark skin tone and skin discolouration.
Sputum collection and analysis: what the nurse needs to know
Rationale and key points Sputum is the term used to describe mucus that has been expectorated. It consists of secretions and other matter that has been coughed up from the lungs and large airways. This article informs nurses about how and why sputum collection and analysis are undertaken. » Sputum is always considered abnormal, because healthy people swallow bronchial secretions. » Sputum analysis is important, because it enables diagnosis of conditions such as pneumonia, tuberculosis, lung abscess and lung cancer. » The nurse should record the colour, amount and consistency of the sputum collected. They should send the specimen to the laboratory for analysis without delay to ensure accurate results.
Measuring peak expiratory flow rate: what the nurse needs to know
The rationale for measuring peak expiratory flow rate and guidance for nurses
Book Review: Respiratory Nursing at a Glance
Rebecca Myatt reviews a book that offers an excellent overview of respiratory conditions.
Nursing and Midwifery Council revalidation
All UK nurses and midwives will be required to perform revalidation as part of their registration process, from April 2016. This entails a pre-determined number of practice hours and study time, reflection on practice, obtaining feedback on individual performance and confirmation of these achievements by a third party source. This article describes the actions nurses and midwives can take to fulfil their revalidation requirements. It also discusses how to prepare for the forthcoming changes and what the nurse and midwife need to consider to perform successful revalidation. By completing the time out activities included with this article, reflecting on your practice and submitting your work for continuing professional development credits, you will be working towards creating a revalidation portfolio, in accordance with Nursing and Midwifery Council guidelines.
Nursing care of patients with a temporary tracheostomy
Safety considerations are important when caring for a patient with a temporary tracheostomy. Early detection and resolution of problems in tracheostomy management are important to prevent serious incidents arising. Nurses working outside critical care areas need to be competent and confident in the management or detection of potential problems with tracheostomies. This article summarises the essential care of a patient with a temporary tracheostomy with reference to best practice guidelines, emphasising the importance of prompt intervention and response, if a potential problem is identified.
Diagnosis and management of patients with pleural effusions
Pleural effusions occur when fluid accumulates between the visceral and parietal pleura in the chest cavity, preventing the lung from expanding fully during inspiration. The reduction in lung volume, depression of the diaphragm and reduced chest wall compliance cause dyspnoea, and occasionally pain or cough. Pleural effusion is a complex problem caused by a variety of conditions requiring different treatment depending on the underlying diagnosis. This article discusses the causes and treatment of pleural effusions, referencing guidelines produced by the British Thoracic Society.
Management of patients with empyema
Empyema is the term used to describe an accumulation of pus in a body cavity such as the pleural space as a result of bacterial infection. The condition is serious because it is difficult for the immune system to resolve infection in this area. Empyema can be avoided by the use of appropriate antibiotic therapy and good aseptic technique when dealing with any situation that breaches the chest wall. Treatment of this condition may be medical but if the condition does not resolve, surgical intervention is required. The nursing role involves providing support, education and long-term management for patients with empyema.
An overview of non-Hodgkin’s lymphoma
Non-Hodgkin’s lymphoma is a heterogeneous group of lymphoproliferative malignancies with differing patterns of behaviour and responses to treatment. Chemotherapy, radiotherapy and stem cell transplantation are the main treatment modalities, but targeted therapies such as monoclonal antibodies are improving survival. The complex nature of the disease, and different treatment pathways, mean that nurses working in this area need in-depth knowledge to provide patient education, continuity of care and advice on current treatment options, as well as to ensure an optimal patient journey.